ACP is dedicated to facilitating research to better diagnose, treat and improve the well-being of those with MS. Exploring MS biomarkers holds great potential for transforming the landscape of MS management, enabling better diagnostics, earlier interventions, and improved symptom control. This research may also reveal more about disease progression, potentially paving the way to targeted therapies and personalized treatments.
What is a biomarker?
The term “biomarker” stands for “biological marker.” Many car owners know the frustration of a “check engine” light flashing on the dashboard. It’s a signal that something’s wrong, but a mechanic’s tests are needed to determine the specific issue. In medicine, a symptom acts like this warning light, alerting you to a health issue, but not explaining it fully. Biomarkers are like the mechanic’s test results; they give doctors detailed information about what’s happening inside the body.

According to the Food and Drug Administration (FDA), biomarkers are “characteristics that are objectively measured as indicators of health, disease, or a response to an exposure or intervention, including therapeutic interventions.”
Some biomarkers are relatively easy to observe, for example blood pressure. Others require more complex testing to detect. Molecular biomarkers have physical and chemical properties that make it possible to measure them in biological samples like blood, or cerebrospinal fluid (CSF, the fluid surrounding the brain and spinal cord). Radiographic biomarkers are obtained from imaging studies. A genetic biomarker (or genetic marker) is a DNA sequence that causes disease or is associated with susceptibility to disease. This month, in the first article of a three-part series, we focus on the molecular biomarkers that are associated with MS.
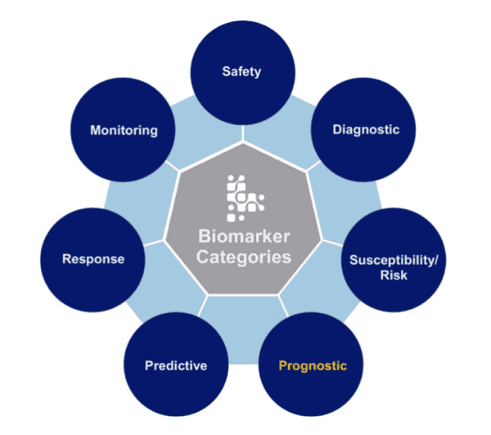
Per the FDA, there are seven categories of biomarkers, each defined by how they are used:
Molecular biomarkers currently used in MS care
Immunoglobulin G (IgG) / Oligoclonal Bands
IgG and oligoclonal bands are diagnostic and prognostic biomarkers for MS. IgG is an antibody usually found in the blood that plays a key role in protecting against bacterial and viral infections. In the context of MS, igG is produced in the CSF. This production indicates that the immune system is active within the central nervous system, a process not typical in healthy individuals. The presence of specific IgG patterns, known as oligoclonal bands, in the CSF is a key indicator of MS. Understanding the production and patterns of IgG in the CSF is essential for learning more about MS and how to treat it.
Neutralizing antibodies are response biomarkers in MS. They are a key indicator of the effectiveness of disease-modifying therapies (DMTs), particularly interferon-beta (Rebif). These antibodies can reduce the treatment’s efficacy by binding to the medication, potentially leading to a loss of response. The development of neutralizing antibodies varies among individuals and is influenced by factors like the type of medication, dosage, and frequency of administration. In clinical practice, regular monitoring for these antibodies is recommended, and their presence may call for changes in the treatment regimen (for example, switching to a different DMT or adjusting dosages). Managing neutralizing antibodies is essential for maintaining the effectiveness of MS treatments and improving patient outcomes.
JC Virus antibodies are a safety biomarker in MS. This index is an important test for people with MS, particularly when they are being considered for certain MS treatments, like natalizumab (Tysabri). The JC Virus index detects antibodies to the JC virus in the blood, indicating past exposure to the virus. The level of these antibodies helps assess the risk of developing a serious brain infection called progressive multifocal leukoencephalopathy (PML). A higher antibody level suggests a greater risk of PML. Therefore, the test is crucial for guiding treatment decisions and facilitates regular monitoring in patients receiving these treatments to ensure the early detection of any increased risk of PML.
CD19 lymphocytes are a type of response and monitoring biomarker in MS. They are found on the surface of B cells, a type of white blood cell that plays a key role in the immune response. In MS, abnormal B cell activity contributes to the disease’s progression and inflammation. Monitoring CD19 lymphocyte counts is particularly relevant when using B cell-depleting therapies, such as ocrelizumab or rituximab. These therapies target and reduce B cells. Tracking CD19 counts provides insight into the extent of B cell depletion and recovery, which is essential for managing treatment.
Emerging MS biomarkers that show promise
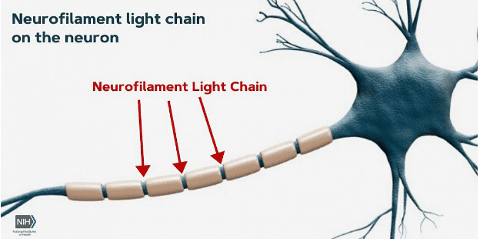
NfL is a protein that is released when nerve cells are damaged. Its levels can be measured in both blood and CSF. In MS, research shows that elevated levels of NfL are associated with more active and severe disease, indicating a higher rate of nerve damage. Investigators in Sweden suggest that NfL can also help to predict future disability and evaluate the effectiveness of therapies. Studies like these provide mounting evidence that NfL may be a valuable tool in both clinical practice and research for better understanding and managing MS.
Chitinase-3-like protein 1 (CH3L1)
CH3L1 is a protein that is produced by microglia. Microglia are a type of cell in the brain and spinal cord that act as “cleaners,” searching for and consuming infectious agents, damaged neurons, or other foreign materials. Microglia “turn on” as part of the body’s immune response. In MS, this activation can lead to inflammation and contribute to demyelination and nerve damage. Elevated levels of CH3L1 in the CSF and blood of MS patients has been linked to increased disease activity, severity, and progression. This association suggests that CH3L1 could be a useful tool for monitoring MS and guiding treatment strategies.
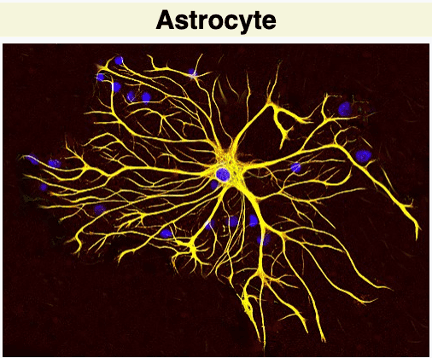
GFAP is a protein predominantly found in astrocytes, which are star-shaped cells in the brain and spinal cord that play a key role in supporting neurons and maintaining the blood-brain barrier. These cells also contribute to scar tissue formation and inflammation. In MS, there is evidence that GFAP levels typically rise in response to disease-related damage, especially during periods of active inflammation and nerve damage. Increased GFAP levels can be measured in blood and CSF samples, making it a possible biomarker for assessing disease activity, monitoring progression, and potentially guiding treatment decisions.

ACP’s wide variety of resources fuels MS researchers worldwide to make more breakthroughs at a faster pace. Through the ACP Repository, investigators can access thousands of existing biosamples, associated phenotypic data and sample analysis data, quickly and at minimal cost. iConquerMS is an 8,500-member strong community of individuals living with MS who are willing to contribute their health data, fresh biosamples, insights and lived experience to advance MS research. These initiatives empower all MS stakeholders to collaborate and move MS research forward.
Researchers at the University of Tennessee used samples from the ACP Repository to explore biomarkers. Want to read more? See the March 2024 Donor’s Corner!