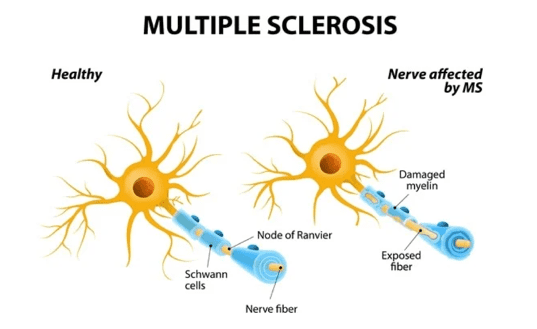
MS is an autoimmune disease in which the body’s immune system attacks the protective covering of the nerve cells in the central nervous system. This causes communication problems between the brain, spinal cord and the rest of the body. Eventually the disease can cause permanent damage or deterioration of the nerve fibers.
The exact cause of MS isn’t known, although experts believe that genetics, environmental, and infectious factors play a role in its development. These factors work in different ways and possibly in combination with each other to determine a person’s overall risk of developing MS.
MS triggers are different for each person. More than 200 genes have been linked to the disease. Being genetically predisposed to develop MS sets the stage for the disease. There are multiple environmental and infectious factors that have the potential to turn these genes on, such as low vitamin D, smoking, obesity and the Epstein Barr virus. Researchers are exploring whether or not head injuries should be added to this list.
Acquired brain injury (ABI) is a broad term that refers to any type of brain damage that occurs after birth. It can have many different causes, including illness, blows to the head, alcohol and drug use or oxygen deprivation.
An ABI that is caused by a blow to the head is referred to as a traumatic brain injury (TBI). There are many different types of TBI, with the most common being a concussion. A concussion is typically caused by a sudden blow or jolt to the head that makes it move rapidly back and forth. This sudden movement causes the brain to bounce around or twist in the skull, creating chemical changes in the brain and, in some cases, the stretching and damaging of brain cells. Concussion symptoms range from mild to severe and, in some cases, can be long lasting. A contusion often occurs alongside a concussion. A contusion is essentially a bruise on the brain, or a mild form of bleeding. Contusion symptoms depend on its size, location and how long it lasts.
Several studies have explored a possible connection between physical trauma and MS, with conflicting results. A 2008 study looked at more than 150,000 Danish men and women less than 55 years old who had been diagnosed with concussion, brain contusion, or skull fracture and hospitalized from the injury.

Researchers determined how many of these people developed MS. They then compared the rate of MS occurring in the head trauma group with people who had MS but no history of head injuries. Data showed no significant statistical difference between the two groups. The researchers concluded that head trauma does not have an effect on a person’s risk for developing MS. In 2013, Canadian researchers conducted a review that analyzed published studies from 1950 onward that had explored associations between traumatic injuries and MS. They also found no significant association between any physical trauma and the development of MS. However, the studies included in this review used varying definitions of traumatic injury, ranging from “accidents and burns” to “head trauma with concussion.” This makes it difficult to definitively rule out a relationship between head trauma and MS.
A 2014 meta-analysis examined 40 studies into the topic of physical trauma and the risk of MS. Results suggest people who experience head trauma and/or other physical trauma as a child (younger than 20 years) and those who suffer head trauma later in life (older than 20 years) have a higher risk of developing MS. No association was found between spinal injury during childhood, or fractures and burns at any age and the diagnosis of MS. The authors called for further research on the topic to confirm these findings.

More recently, a 2017 study used data from the Swedish National Patient Register and Swedish MS Registry to identify 7,292 individuals with MS. Each person with MS was individually matched by sex, age, and place of residence with 10 people who did not have MS.
The team identified any diagnosis of concussion among participants during childhood (between birth and the age of 10 years) and adolescence (between the ages of 11 and 20 years). They found no association between concussion in childhood and the risk of MS in later life. However, results showed that participants who experienced one concussion in adolescence were 22 percent more likely to receive an MS diagnosis later in life, while the risk of MS more than doubled for those who suffered more than one concussion as a teenager. To rule out the possibility that general physical trauma might lead to MS, they also compared broken limb bones between the two groups. There was no connection between broken arms or legs and the risk of MS. It’s important to note that these conclusions are based on data from a limited population. Additional studies looking at more diverse groups of subjects are needed to further validate them.
There are several theories for how head trauma could contribute to a person developing MS. There is evidence that a head injury triggers an autoimmune response that impacts the blood-brain barrier. This is the border of cells that lets substances in and out of the central nervous system.
If a head injury affects this barrier, substances that are usually blocked could enter the brain and spinal cord, including myelin-attacking cells. Other potential mechanisms through which concussions and other TBIs could lead to the development of MS include damage to the nervous system tissue itself (which may lead to an inappropriate immune response). Head trauma also has the potential to set off a state of inflammation in the brain that could predispose a person to MS.
While there is evidence that head injury may increase the risk of developing MS, there are limitations in the research that has been done to date. Past studies have used different study methods, varying definitions of head trauma and included a limited sector of people. This makes it difficult to make a firm connection between head trauma and MS. More research is needed using consistent parameters and looking at more diverse populations to shed light on this topic, and to determine how trauma might trigger an autoimmune disease like MS. The core of ACP’s mission is to facilitate research efforts into topics such as these, which have the potential to improve the health and quality of life for people living with MS throughout their lifetime.

